I’m going to cut straight to the chase with some numbers.
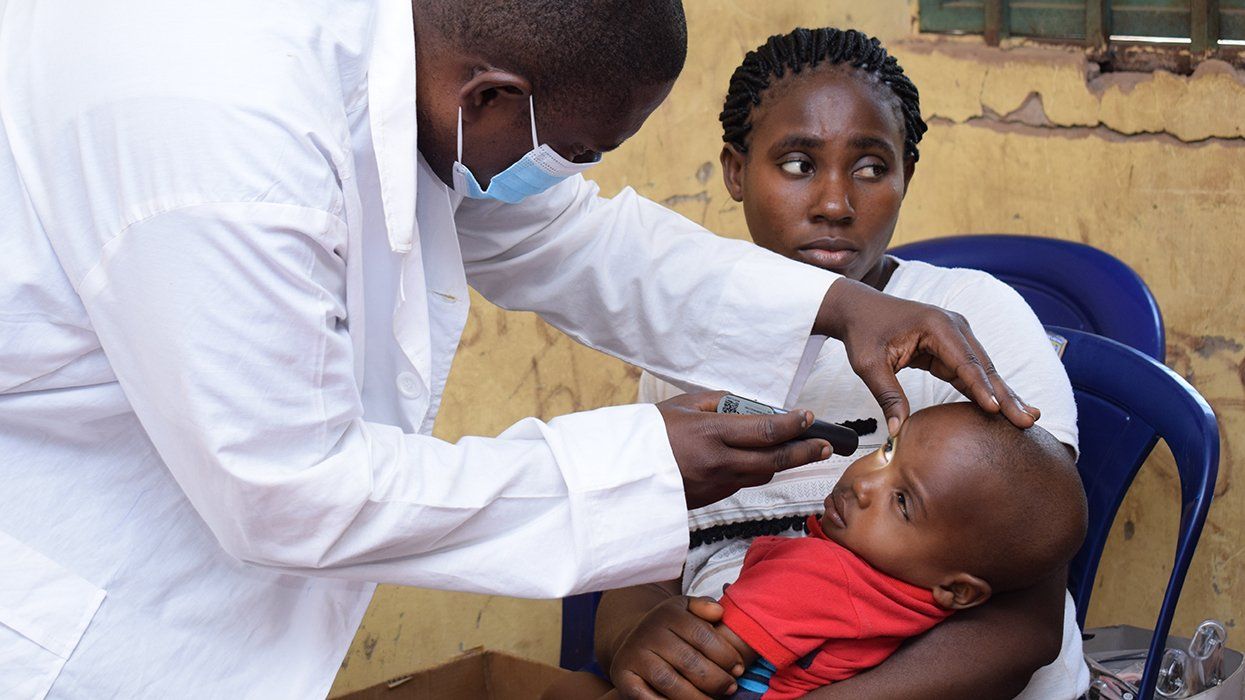
Over half of HIV-positive people in the world are women. Globally, the greatest cause of death among women ages 15-49 is AIDS-related complications; AIDS diagnoses have disproportionately tripled among women in the last 30 years.
In Sub-Saharan Africa, women ages 15-24 now account for 75 percent of all new infections. Young women in sub-Saharan Africa are eight times as likely to be HIV-positive as men.
The majority of women who contract HIV do so through heterosexual sexual contact and, in many cases (like 90 percent of women in Asia, for example) their husbands infected them after marriage.
There is one common denominator to all of these stats: Gender-based violence.
It’s is the No. 1 precursor to a woman being infected with HIV. Right now at least 1 in 7 new infections in women can be directly attributed to either male partner violence or women’s lack of relational power; generally their main “risk factor” is having sex with their primary male partner, which means they fall outside of every parameter of who has been traditionally targeted as an “at-risk” group. But make no mistake; women survivors of abuse are an “at-risk” group.
It's time to talk about violence.
I’m not the first to say this but it bears repeating: globally, HIV is now a gender-based disease; spread by men, but suffered by women. And that is because of the high rates of gender-based and intimate partner violence aimed at women, and the way in which it greatly exacerbates HIV risk.
Women and girls who have experienced violence have a substantially increased risk of HIV infection, a risk that is both increased directly through sexual violence or indirectly through increased risky behavior or inability to negotiate safer-sex practices with a partner.
Women abuse survivors are in double jeopardy, as well: they are more likely to be infected by an abusive partner and then once positive, more likely to become a target of abuse. Consider these stats of women in the U.S.:
• In the U.S., more than a third of women have experienced gender-based violence; of those 91 percent were under 25 years old.
• Over half of women with HIV (55 percent) have experienced violence; that's nearly double the national average of 36 percent.
• Transgender women experience violence at even higher rates — 58 percent — and among trans women of color, there are even more alarming rates of HIV infection.
• One in 5 HIV-positive women reported experiencing violence after they became positive; half of them attributed that violence directly to being HIV positive. (Reports show the numbers of post-positive violence is even higher in African countries where stigma and misinformation are commonplace.)
Indeed, internationally the numbers are even worse. In the last decade, wide-scale studies across Asia and Africa have shown women who experience violence from male partners are significantly more likely to be infected with HIV.
In some African countries, intimate partner violence is around 48 percent; the mortality rate from IPV in South Africa is double that of the U.S.
In South Africa, 44 percent of men admit to physical violence against their female partners, and intimate partner violence is so common that in one study, a majority of high school students surveyed in the country said they did not consider forced intercourse a crime.
But surely, you may say, violence is just one risk factor among many.
Not really. If you look at the risk factors like drug use and sex work and so on, you'll see many, if not all, can be linked back to childhood abuse, sexual assault, or domestic partner violence. For example, women who experience gender-based violence are more likely to report risk factors like unprotected sex, IV drug use, and alcohol abuse. Early sexual violence as a child affects a woman’s HIV risk throughout her life through increased likelihood that she will become involved in an abusive or controlling relationship, which has been proven to increase HIV risk.
Studies in Rwanda and Tanzania — in fact study after study since 2004 — show that HIV-positive women were more likely to report a history of physical violence, sexual coercion, or gender inequality because women subjected to those forms of violence are less likely to request condom use, more likely to have partners who have risky sex behaviors outside their relationship, and more likely to have genital tract injuries associated with sexual violence (which increase HIV susceptibility).
And once those women seroconvert and are HIV-positive, they are less likely to get treatment, more likely to go off their medication, and to miss health care appointments. Even in the U.S. where access to medical care and medication are much easier than in other parts of the world, only 41 percent of women living with HIV are retained in medical care. You’ve read the headlines earlier this year about the baby once thought functionally cured of HIV? The only way the doctors were able to make that breakthroughs is because the mother had stopped getting care for her own HIV for a time and finally came back to the doctor for the sake of the child.
Men are the root of the problem and men must be a part of the solution. We cannot solve this without them.
In honor of Domestic Violence Awareness Month this month, the Positive Women's Network-USA spearheaded a National Day of Action to End Violence Against Women Living with HIV. That's today. Both events are like National Women and Girls HIV/AIDS Awareness Day, in that they all serve as a great reminder that any resolution to the problem of women and HIV belongs not just to governments, and public health workers, or non-profit organizations, but to people like us. And violence is a problem.
While there are a number of things we need to do, the first is to include men in the solution. The links between violence, inequality, and risky behavior are clear, but more must be done to find ways to reduce each of them.
Research on working men in South Africa, married men in India, and men in methadone treatment programs here in New York who admitted to being perpetrators of intimate partner violence found that this disparate group of men were all far more likely to report multiple sexual partners, thus increasing their risk for HIV, and some researchers have postulated that abusive men are more likely than non-abusers to be HIV positive or to be infected with co-factors like genital herpes, which make women more vulnerable to HIV transmission.
How do we combat that?
First, with strong national and international leadership condemning intimate partner and gender-based violence, and with programs that engage men in ways to prevent gender-based violence while encouraging them to also adopt HIV prevention strategies.
Altering gender-based abusive behaviors and sexual risk behaviors of men is not a pipe dream. There’s a pilot program in South Africa that targeted young men, which successfully found reductions in both risky sexual behavior and abusive behavior. Every community needs a program like this tailored to their own area’s cultural needs. Men who are violent are trapped in their own cycles that we need to uproot. It can be done.
We must do this by empowering women, too.
It can’t just be about fixing male behavior. We need to push governments, health officials, scientists, and organizations to empower women by these small steps:
• Create more discrete ways to test and treat HIV around the world, including, where possible, routine physician screenings. Imagine if HIV testing was as routine as a pap smear or a cholesterol test? In countries where health care is limited, placing primary care workers in villages around that country could also serve this purpose.
• Increase intimate partner violence screening and HIV testing for girls and women and encourage concurrent screening where possible.
• Train domestic violence counselors on the links between HIV and violence and encourage them to promote testing and HIV risk reduction. Train HIV clinics in how to spot and deal with incidents of abuse, as well. These two types of resources are the front lines; imagine if they could work with each other to bring these numbers down?
• For transgender women, collaborate with LGBT service organizations to do all of these things above better for trans women.
• Find better ways to address lifecycle trauma (since we know its associated with treatment failure) and develop and implement models that integrate trauma care with HIV screening/treatment.
• Address females at all life stages. Too often, because it’s an safe political sale, we focus on prevention or care for women who are mothers or pregnant women with HIV and while those groups do need care, motherhood is only one part of a woman’s complete lifecycle in which she is susceptible to HIV. Many women who contract HIV will never be mothers, by choice or circumstance.
• Develop more programs (leadership training, microfinancing, etc.) that add to women’s economic resources, confidence, and ability to gain shared decision-making power. Microfinance programs, for example, offer economic independence and strengthened social networks. Once women are economic contributors to their households they are often better able to challenge inappropriate sexual roles and abusive behaviors.
• Develop more female-controlled methods of HIV prevention. Anyone who wants to stop HIV among women should be putting a ton of energy into a vaginal microbicide.
• Demand leaders throw their political weight behind expanding sexual and reproductive health services, legislating (and enforcing) gender equality, and ending violence against women.
• Strengthen school-based HIV prevention and education programs everywhere.
• Change existing HIV reporting laws and decriminalize HIV. Criminalization laws contribute to climate of fear and stigma while laws that require disclosure can make women even more susceptible to intimate partner violence. Laws need to account for circumstances where disclosure of HIV status may subject the disclosing partner to violence.
Most of all...
We need to to this work across multiple platforms — within health care, employment, law, and media — and address all facets of gender-based violence (child molestation, intimate partner violence, rape, etc.) to make sure everyone understands the scope of the intersection between HIV and violence against women and girls and is equipped to combat it.