Treatment
Viral Maps Show Exactly How An HIV Outbreak Spread

Epidemiologists were able to "ask" the HIV virus itself how it spread in an innovative new approach to tracking outbreaks.
January 26 2018 10:15 AM EST
By continuing to use our site, you agree to our Privacy Policy and Terms of Use.

Epidemiologists were able to "ask" the HIV virus itself how it spread in an innovative new approach to tracking outbreaks.
Epidemiologists traditionally have depended on what people say to discover how disease spreads. But in investigating Indiana's recent HIV outbreak, the CDC tracked what the virus says — by looking at its DNA.Scientists at the Centers for Disease Control and Prevention used a novel disease-mapping method to study how HIV spread during the 2015 outbreak in Scott County, Indiana. The outbreak struck 227 people in this small rural county, and was mostly transmitted through injection drug use. A report in the Journal of Infectious Diseases summarizes the agency’s findings, including the fact that most people connected to the outbreak were infected before the state declared a public health emergency.
CDC Computational biologist and lead author Ellsworth Campbell said because HIV mutates over time, researchers can compare samples of the virus’ DNA and deduce who spread the virus to whom. How different viruses are from each other can indicate how recently someone has been infected. The CDC used blood samples that were collected in the field to analyze Scott County residents' HIV sequences and their "genetic distance" from each other.
“We used that to get an idea of whose viruses are so similar that they really had to be linked by recent transmission —maybe not direct transmission — but they may be one hop away, for example,” Campbell said.They then connected that data with on-the-ground interviews with HIV-positive people, placing the “maps” of transmission information on top of each other.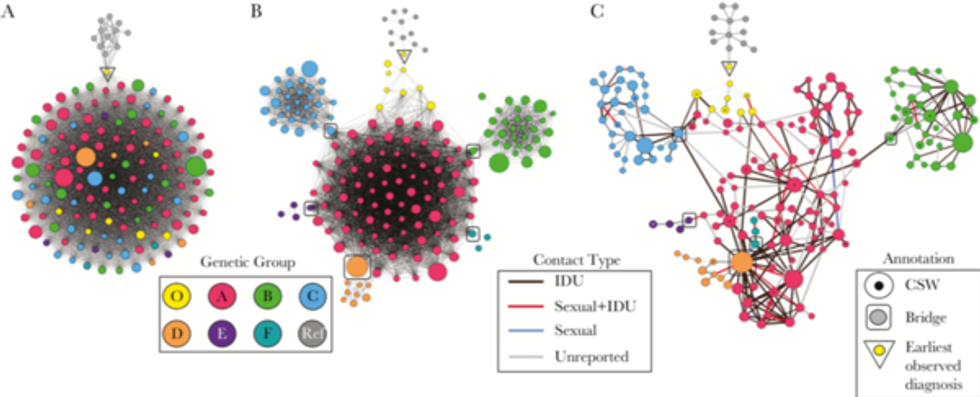
The new approach gave public health officials previously unknown insights into the epidemic. Campbell said that data showed the virus existed in the area for nearly a decade before transmission exploded, and the initial patient wasn’t an intravenous drug user. However, once the virus started spreading through drug use, the HIV rate exploded.
“What this told us is there were a handful of sub-outbreaks that stemmed from a single case that was diagnosed about ten years ago,” said Campbell.
The authors point out most transmissions occurred before the state declared a public health emergency, which paved the way for a sterile syringe services program, or needle exchange. After that declaration, Campbell says, the outbreak was largely contained.
The authors said that should serve as proof needle exchanges can prevent future outbreaks.
“It didn’t tell us anything new, but it confirmed what we had expected,” said Brittany Combs, a public health nurse with the Scott County Health Department who operates the county’s syringe services program.
Combs said county health officials saw firsthand the work the CDC was doing when they visited the agency’s headquarters in Atlanta during a 2015 HIV conference.
She said when she saw the team’s visualizations of the data — a map of tangled dots and lines that showed how infected people were connected — it looked familiar. The clusters of dots lined up with known groups of drug users.
“[We said], we think this is exactly where this group of people was hanging out and sharing needles, and you can kind of see where it’s connected … and then there’s this other group. We could pinpoint it down to the house,” she said.
Both she and Campbell said the new blend of research methods could help understand other outbreaks and prevent them from getting worse.
“We put a human aspect on it, and then they had the numbers aspect,” said Combs. “When you combined both of them, you could see how it spread through this tight-knit community.”
This story was produced by Side Effects Public Media, a reporting collaborative focused on public health.